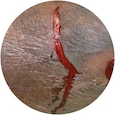
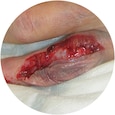
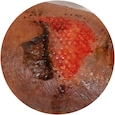
“Skin tears represent more than one in ten wounds in skilled nursing facilities.”1 They are an often-misunderstood issue and can become a serious problem if not treated correctly.
When a skin tear occurs, a comprehensive approach to treatment is required. The selection of wound care products depends on individual patient needs and is crucial for successful wound healing.
Silicone-based dressings allow for atraumatic removal, ensuring that fragile skin is not further harmed. That’s why we recommend you try Leukoplast skin sensitive – a very comprehensive range of silicone-based dressings.